Ethical notice: This article is for educational purposes only and does not replace medical advice. If you have persistent symptoms, significant family history, anemia, or abnormal tests, seek individualized medical evaluation.
Why this guide exists
Colon cancer is one of the most common cancers worldwide—and one of the most preventable. Many cases develop slowly from polyps over years. That creates a powerful window of opportunity: if you remove precancerous lesions early, you can interrupt the disease process before cancer develops. And when cancer is found early, treatment is often simpler and outcomes are typically better.
This is a top-of-funnel, “start here” guide built for clarity. You will learn:
- What colon cancer is (and why it often starts as a polyp)
- Symptoms that deserve attention (and what people often dismiss)
- Who is at higher risk
- How screening works—and why it saves lives
- How diagnosis is confirmed
- What happens after diagnosis (staging and treatment basics)
- When to seek specialist input (including peritoneal oncology)
If you’re looking for a deeper, more advanced topic (peritoneal metastases, CRS/HIPEC, PCI, staging challenges), I included a cluster map at the end so you can build a full learning pathway on Peritoneo.life.
What is colon cancer?
Colon cancer (often grouped with rectal cancer as colorectal cancer) is a malignant tumor that arises in the large intestine. In many people, it begins as a benign growth called a polyp. Over time, some polyps can evolve into cancer. This is why colonoscopy is such a central tool: it can both detect and remove many precancerous lesions during the same procedure.
Key idea: colon cancer is often not a sudden event. It frequently develops through stages, and screening aims to catch the process early—before symptoms appear.
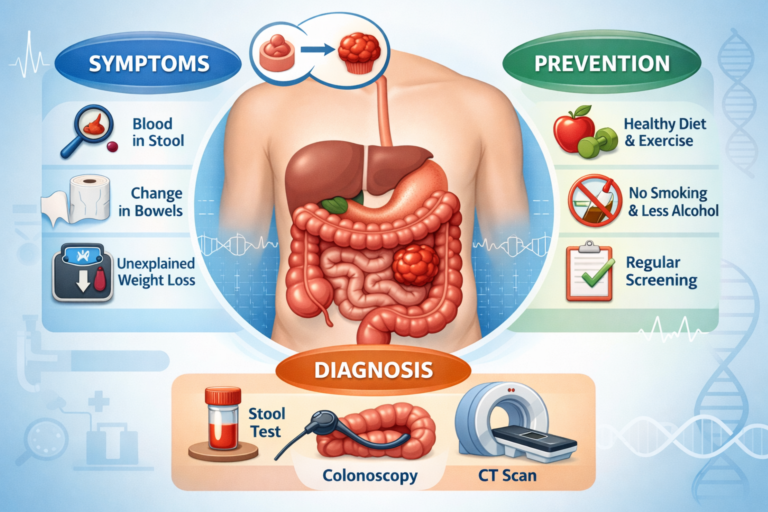
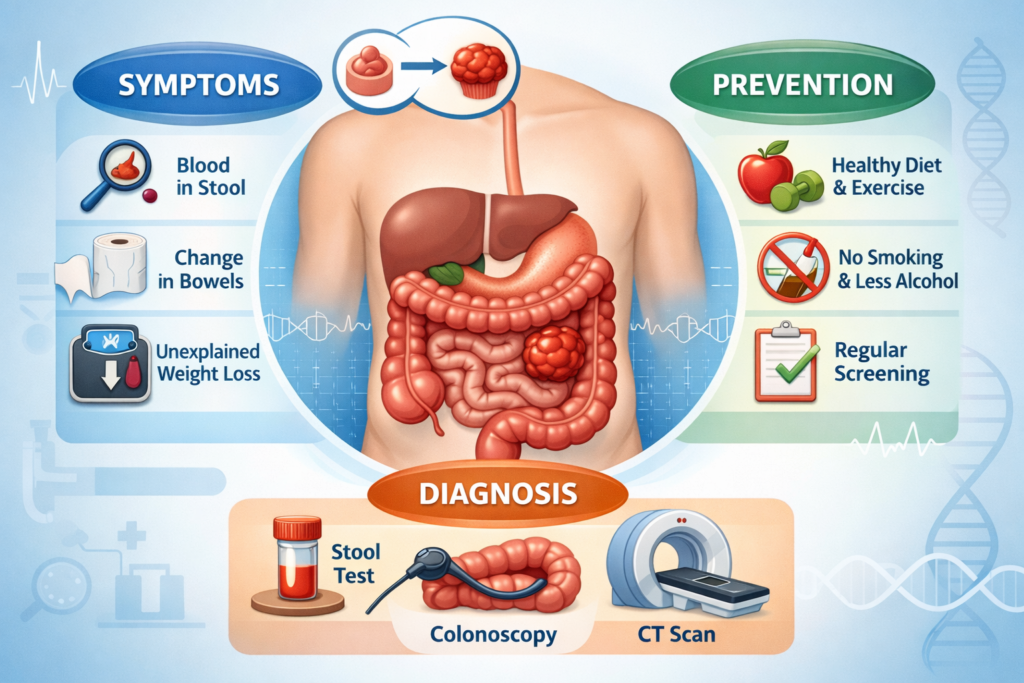
Symptoms: what you should not normalize
Not every symptom means cancer. But several symptoms deserve medical evaluation—especially if they persist for more than 2–3 weeks or occur together with anemia, weight loss, or declining energy.
Common warning signs
- Blood in stool (bright red or darker/blackish stool)
- Persistent change in bowel habits (new constipation, new diarrhea, alternating patterns)
- Narrower stools that persist
- Abdominal pain that is new or recurrent
- Bloating or progressive abdominal distension
- Feeling of incomplete evacuation
- Unexplained iron-deficiency anemia
- Unintentional weight loss
- Persistent fatigue that is new for you
- Signs of obstruction (severe pain, vomiting, inability to pass gas/stool)
A practical rule
If you are treating “hemorrhoids” repeatedly but the bleeding persists, or if you have anemia, weight loss, or worsening symptoms, don’t settle for assumptions. Ask for a structured diagnostic plan.
Who is at higher risk?
Risk is not equal for everyone. Certain factors increase the likelihood of developing colon cancer—and influence when and how aggressively screening should occur.
Higher-risk factors
- Family history of colon cancer or advanced polyps (especially in first-degree relatives)
- Personal history of polyps or colon cancer
- Inflammatory bowel disease (ulcerative colitis or Crohn’s disease involving the colon)
- Hereditary syndromes (e.g., Lynch syndrome, familial adenomatous polyposis)
- Lifestyle factors (obesity, low physical activity, smoking, heavy alcohol use, diets high in ultra-processed foods)
- Age (risk increases with time, but younger-onset colon cancer has become more visible in recent years)
Important: If you have meaningful family history, screening often starts earlier and follows different intervals. This must be personalized.
Screening: why it saves lives
Screening means testing people before symptoms appear. In colon cancer, screening can prevent cancer by removing polyps—and it can detect cancers earlier when treatment is more effective.
How screening is done
Screening strategies vary by country and guideline. The two common pillars are:
- Stool-based tests (looking for hidden blood or tumor DNA signals)
- Colonoscopy (direct visualization with the option to remove polyps and biopsy lesions)
Which test is “best” depends on your risk profile, local availability, and medical history. A good plan is the one you will actually follow—and that fits your risk.
Diagnostic workup: what typically happens when cancer is suspected
If symptoms or screening tests raise concern, clinicians usually move to confirmation and staging.
Common steps
- Blood tests (CBC, iron studies, liver function, inflammatory markers as appropriate)
- Colonoscopy (with biopsies if a lesion is found)
- Pathology (to confirm diagnosis and define tumor features)
- Imaging (CT or MRI to evaluate the extent of disease; additional studies depending on the case)
Practical tip: If you already had a colonoscopy, keep the report and photos, the pathology results, and any imaging CDs/links. Good documentation speeds up decision-making.
What happens after diagnosis: staging (in plain language)
Staging describes how far the disease has spread. It guides treatment choices and helps teams estimate prognosis. Even without diving into technical details, here is the core idea:
- Early-stage disease is typically limited to the bowel wall and nearby structures
- Locally advanced disease may involve deeper layers, lymph nodes, or adjacent organs
- Metastatic disease means spread to distant sites (commonly liver or lungs, but also the peritoneum)
Most patients benefit from multidisciplinary discussion—especially when decisions include surgery, systemic therapy, or specialized approaches.
A critical advanced topic: when colon cancer involves the peritoneum
In a subset of patients, colon cancer can spread to the peritoneum (the lining of the abdominal cavity). This is commonly called peritoneal metastases or “peritoneal carcinomatosis.” It often behaves differently from liver- or lung-only metastases and frequently requires specialized staging and specialized decision-making.
If you suspect or already know peritoneal involvement, this is where peritoneal oncology expertise becomes essential—because the first decision often determines what treatment options remain viable.
CTA (lead capture): If you want to organize your diagnostic pathway or seek a second opinion, subscribe to the Peritoneo.life updates and request our specialist pathway resources.
What you can do today to lower your overall risk
No single habit is a guarantee—but a set of consistent behaviors reduces risk and improves overall health:
- Maintain a healthy body weight
- Increase dietary fiber and reduce ultra-processed foods
- Exercise regularly
- Stop smoking
- Moderate alcohol intake
- Prioritize sleep and stress management
- Follow a screening plan that matches your risk
Frequently asked questions
Does colon cancer always cause symptoms?
No. Early disease can be silent. That’s why screening is so powerful: it aims to catch polyps and early cancers before symptoms appear.
Is blood in stool always cancer?
No. Hemorrhoids and fissures are common causes. But persistent bleeding—especially with anemia, weight loss, or change in bowel habits—should be investigated.
Is colonoscopy the “best” test?
It is one of the most comprehensive tests because it can detect lesions and remove polyps during the same procedure. The best screening test is the one matched to your risk and performed on schedule.
If I have a family history, should I screen earlier?
Often yes. The right age and interval depend on your relative’s diagnosis age, degree of relation, and your own medical history.
Can colon cancer be cured?
Many cases can be cured—especially when detected early. Even with advanced disease, modern multimodal strategies can offer meaningful control, and selected patients may have long-term outcomes with specialized treatment pathways.
Can colon cancer spread to the peritoneum?
Yes. Peritoneal metastases can occur and often require specialized staging and treatment strategy planning.
What symptoms require urgent evaluation?
Severe abdominal pain, persistent vomiting, inability to pass gas/stool, significant bleeding, fainting, and signs of dehydration should be treated as urgent.
How do I prepare for a specialist visit?
Bring symptom timeline, family history, medication list, colonoscopy report, pathology results, and imaging studies. Good documentation saves weeks of delay.
Don´t wait anymore
If you have persistent symptoms, anemia, a strong family history, prior polyps, abnormal screening tests, or a new diagnosis and want a structured plan, we can help you organize the next steps.
Subscribe to Peritoneo.life: https://peritoneo.life/newsletter/
Request specialist pathway resources: https://api.whatsapp.com/send/?phone=5512988004037